Around 2 million Canadians suffer from depression every year. For some, even multiple cycles of antidepressant dosage fail to help. 4,500 Canadians die by suicide annually according to the Canadian Vital Statistics Death Database (CVSD).
We are in need of a well-founded solution to the alarming increase in mental health struggles among our youths, and ketamine may be the start of what antidepressants couldn’t do. With the discovery of ketamine in treating depression, a study done by Yale Medicine suggests that it has the potential to be the first step to developing more effective ways to deal with future mental health stressors and prevent possible relapses.
But there is still much research to be done on Ketamine and its possible side effects on the human body. By now, we know as much as it must strictly be used under the prescription and surveillance of a medical expert. This blog post will walk you through everything you need to understand about ketamine.
What is Ketamine?
The Center for Addiction and Mental Health (CAMH) defines ketamine as, ‘a fast-acting painkiller and anesthetic.’ It is a type of drug that can make one experience vivid illusions and disorient oneself from their body and consciousness. Because of its quick and strong effect on changing brain receptors, it can help with pain management, and be used as an anti-inflammatory, or antidepressant agent. However, because of its excessive side effects, lack of pure knowledge, and addictive nature, it is strictly restricted from consumption without an expert prescription and monitoring.
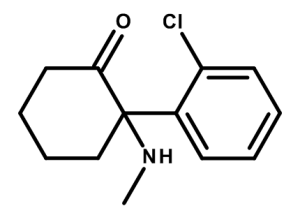 Molecular structure of Ketamine (C13H16ClNO)
Molecular structure of Ketamine (C13H16ClNO)
How does it work?
Ketamine changes the course of one’s brain to feel and experience a different reality. In other words, it utilizes the neuroplastic ability of the brain to change what you were initially thinking, feeling, or perceiving as reality.
In simple terms, Neuroplasticity is the ability of our brain to change its activity by reorganizing its structures, or functions. As the term itself suggests, the ‘neurons’ of our brains can be changed and are malleable, just like ‘plastic’.
Naturally, the plasticity of our brain is able to change over time to adapt to external influences and cope. We can relate such a phenomenon to a possible outcome of a traumatic brain-injurious accident where one may lose a certain grip on what’s real and what’s not. We have the capability to suddenly change our thoughts by evolving and adapting to new needs.
Ketamine is an added external factor that rapidly changes the neuroplasticity of our brains. For instance, when one is being operated on, the Ketamine used as anesthetic changes the feeling of pain into something wholly different for a certain period of time.
History of Ketamine
Ketamine was discovered in the 1960s, and scientists have been baffled by its capabilities ever since. The drug is still under experimentation to understand it’s possibilities in revolutionizing the chronic mental health treatment systems.
Early Discovery Phase
It was in 1956 when phencyclidine was invented as a general anesthetic for pain management in the operation theatre. But scientists later discovered that the chemical had a multitude of side effects even after the surgery, and soon it was banned from being used at all. Instead, they refined it to be a faster-acting and short-term anesthetic. After multiple attempts, ketamine was discovered in 1962.
Use of Ketamine in Human Anesthetic
The first human to receive ketamine was in 1964. Researchers found the effect of the drug led people’s consciousness to disorient their bodies, not feel any pain, and reach a euphoric state of mind. After a continuous success rate, ketamine made it to the market as a ‘dissociative anesthetic’; where one disassociates from reality. Fast forward to the 1970s the US Food and Drug Administration (FDA) approved Ketamine as a general anesthetic in the operating room.
Reclaim your power and heal with our expert counselling services.
Call Thrive now, and take back the control of your life.
Ketamine as a Pain Management Agent
It was when the Vietnam War (1955 – 1975) was happening. At the time, Ketamine started being consumed for pain reduction for war veterans. In fact, because of its ability to quickly disconnect the individual from the pain and trauma of the war, it became widely popular as sedation. Its application continued until the 1990s. It was the decade when procedural sedation started being done with the use of ketamine throughout hospitals in different parts of the world.
A Breakthrough for Antidepressants
In 2000, Yale University published a study on the use of Ketamine as an antidepressant agent. After years of research, by 2012, scientists believed this was the very first effective treatment for severe depression, and could possibly be used to treat severe suicidal thoughts, OCD, PTSD, anxiety, and other mental health problems. Till the present, with the right amount of usage under an expert medician’s supervision, the outcome has become successful to treat hundreds of patients. Yet, more research is needed as overdose and unsupervised consumption can have harmful side effects.
Medical & Therapeutic use of Ketamine
While ketamine is a registered drug for anesthetic, its therapeutic use is still in its initial stage. Putting its side effects in hand and their consequences, monitored doses of ketamine have various applications.

Anesthesia
Ketamine is commonly used as anesthesia in the operating room. It is popular as a sedation in operation procedures like fracture surgeries, fixing bone dislocations, in the treatment of wounds, etc.
Pain Management
As we talked about earlier, ketamine has a history of being used for pain management. It can change the neurons that feel pain in one’s brain into something else. However, it is only used under strict supervision for extreme chronic pain like neuropathic pain, cancer pain, migraines, or burns.
Depression and Anxiety Treatment
Ketamine is also used for cases of depression that failed antidepressants. For instance, it can help a severely depressed patient to change the dimensions of their feelings into something completely different through the ketamine effect.
PTSD Therapy
With its ability to change the discourse of a thought, ketamine can also be incorporated into the treatment for rare severe cases of PTSD. It can displace the brain neurons that ‘carry’ the traumatic experience and replace it with another feeling.
PTSD in War Veterans
In some cases, medical practitioners have used ketamine on war veterans to help them through the trauma of the war itself. The drug is paired with other PTSD therapy procedures to help the veterans relocate their memory of the war from a different angle.
How does Ketamine work for Depression?
Ketamine therapy is done for depression patients who were not able to get better with antidepressants. On one hand, antidepressants increase neurotransmitters in our brain, i.e. changes the signal that determines mood and emotion in our brain. For instance, with its appropriate dosage, one’s emotions can change from sadness to happy emotions. Ketamine, on the other hand, works in a whole different system of the brain.
The neurons in our brains are interconnected with each other. Severe depression directly decreases that interconnectedness, leading to detachment or withdrawal. Ketamine is used to enhance the connection by changing the course of the neurons. Rather than changing the transmission or signaling of emotions like antidepressants, ketamine changes the emotion entirely.
The thoughts one was having before are completely transformed into something else. It can be seen as a resilience mechanism in our brains. For instance, if one was thinking of taking their own life, this therapy can change the course of their thoughts and experiences and completely replace the self-harm thoughts with something else.
However, ketamine treatment is not complete without other therapy methods like psychotherapy. When a patient is treated with ketamine, they lose their initial train of thought to something completely different. They need psychotherapy to help them adapt to the change and understand what happened. This is to prevent reaching back to ground zero after the drug wears off, and help them live with the new reality.
The Most Common Side Effects of Ketamine
Ketamine is restricted to consume without the prescription and presence of an expert as it has extreme adverse side effects when abused.

- Nausea/vomiting
- Dizziness/drowsiness
- Confusion
- Euphoria/dysphoria
- Hallucination
- Poor mind and body coordination
- Allergic reaction (mild and serious)
- Muscle stiffness/spasms
- Seizures
- Feeling of disassociation
- Anxiety from disorientation
- Respiratory problems
The Potential Risks of Ketamine
Regardless of its benefits with certain medicinal procedures, ketamine is a harmful hallucinogenic drug that carries extreme risk.
Physical Effects
Due to its extremely powerful anesthetic nature, there is a potential for widespread physical effects with ketamine.
Instability of Heart and Blood Vessel Function
There is a high chance of fluctuation of the heart rate and abnormal heart rhythms. It also directly affects blood pressure by temporarily increasing and decreasing. In sensitive cases, it can cause a cardiac arrest or a heart attack.
Liver Damage
Especially for patients with past health problems in their liver, the use of ketamine can cause liver damage or dysfunction.
Respiratory Depression
In some cases, patients can’t help breathing extremely slowly, specifically when there is a history of respiratory problems.
Physiological Effects
Often, the use of ketamine can cause extreme delusions and hallucinations. In the long term, high dosages can end up in cognitive function problems like issues with their memory, decision-making, contemplation, and attention skills.
Addiction and Abuse
One use for treatment can lead the patient to abuse the drug to feel better again. With frequent use of ketamine, one can easily fall into addiction. Extreme addiction and abuse may further enhance other potential risks and cause them more harm in the long run. One may start distorting from their own reality and detached from themselves and their body, causing further mental health problems.
The Dangers of Ketamine Overdose
Ketamine overdose includes an extremely large consumption of the drug compared to the amount used in medicinal treatment. While it has its long-term effect, overdose can lead to sudden and life-threatening consequences. Ketamine becomes dangerous when it is mixed with alcohol or other forms of recreational drugs as well. A large amount of ketamine can lead to extreme disorientation in the body, causing the person to breathe extremely slowly. If it continues without emergency medical care, the outcome has a possibility of being fatal.
The Legal Status of Ketamine in Canada
In Canada, ketamine falls as a Schedule I drug in the Controlled Drugs and Substances Act (CDSA). Therefore it is prohibited for market sale, possession, distribution, and consumption without prescription and expert supervision.
A scientifically proven safe and adequate quantity can be prescribed by a licenced medical expert as an operating room anesthesia or chronic pain. It can also be legally a part of mental health therapy for extreme cases like treatment-resistant depression. Although, it is important to note that ketamine has only been FDA-approved for general anesthesia, while its other usage are still under research and haven’t been officially approved yet.
Receiving Ketamine and Coming Back to Real Life

In most case scenarios, ketamine therapy can last for up to 40 minutes to an hour. A comparatively low dosage is used for sedation as compared to other sedation drugs. The patient is given tablets to dissolve in the mouth as well as through intramuscular injection. In some cases, it is used with other anesthetics or, for depression, it may be used with antidepressants. It is done under the supervision of a licenced professional. For more severe cases, the session may be repeated over the course of a couple of weeks, while some need lesser treatment procedures.
Doctors recommend resting for the rest of the day to prevent the remaining drug substances in the body from affecting daily activities. Often, the result of depression treatment is seen rapidly as the drug starts working immediately. It is then combined with other procedures of psychotherapeutic treatment to help the patient keep up with the change and avoid disorientation from their reality.
Safety Measures when using Ketamine
It is significant for the medicinal practitioner to take care of all safety measures when providing ketamine. It is also necessary to understand the procedures and be self-aware when deciding on a treatment from the patient’s end.
Here are some safety measures when using Ketamine:
- The medical practitioner must be licensed, qualified, and experienced.
- The medical centre must be equipped with all necessary and potential aspects.
- The patient must be consented to and briefed about the process and potential side effects they may experience.
- The practitioner must supervise the treatment throughout.
- The patient must be given post-care and followed up on time for the next treatment.
- The patient shouldn’t be given access to or consume ketamine when they are on their own.
Conclusion
At present, we can already witness lifelong treatment-resistant depression patients finally recovering with proper ketamine therapy. With the awareness of all side-effects and risks, proper dosage and expert supervision can revolutionize the rising mental health and suicidal rates in Canada. With all that said, it is eminently important to be cautious and stay under expert advice to avoid any form of the negative outcome. After 50 years of trial and error, we are finally at a time where reliable supervision can save lives with this therapy technique. With all that said, we need more research and experiments to utilize the possibilities of ketamine and hopefully much safer variants in the future.
Remember, you are not alone; help is available. Reach out to Thrive’s Vancouver Counselling Centre for support and guidance without hesitation.
Get Help Now – Call Us at 604-227-0297
Ketamine FAQs:
Is Ketamine Addictive?
Yes, with frequent heavy doses, ketamine can be extremely addictive because of its pain-relieving and hallucination effects.
Is Ketamine an Opioid?
No, ketamine is not an opioid. Opioid works in the opioid receptor in the brain, while ketamine works with multiple receptors like the NMDA receptor (N methyl D aspartate). An opioid is specifically a pain medication, while ketamine is a hallucinogenic anesthetic with a much vaster effect on the human body.
What is Ketamine made of?
Ketamine, or Ketamine Hydrochloride, is made up of many ingredients like Citric acid, Silica gel, Stevia, Acacia, and Polyethylene glycol 1450.
What is Ketamine Therapy?
Ketamine therapy refers to the treatment of resistive mental health issues by the incorporation of ketamine with other therapy methods. Learn More!
How long does Ketamine last?
On average, ketamine can last from up to 20 minutes and 1 hour.
How much Ketamine should I take for depression?
When treating depression with ketamine, it is mandatory to be under the prescription and supervision of a licensed medical expert. They must first test your state of depression, and your history with it, and then only determine whether ketamine is needed or not. You will be given the right amount of dose by your doctor under their care and they will decide on the number of treatment sessions based on your case.
Carson Kivari is the Founder and Clinic Director of Thrive Downtown, with years of experience helping individuals and couples overcome anxiety, depression, and burnout. He guides clients on a journey of self-exploration and trauma release to find purpose, connection, and safety. Take the first step towards healing and contact Carson today to schedule a session.



